Best Age to Get Pregnant with PCOS

Last Updated on March 27, 2024 by Avi Steen
Navigating the journey of pregnancy can be a bit like solving a tricky puzzle, especially when you’re dealing with PCOS (Polycystic Ovary Syndrome). It’s like trying to find the perfect time to jump into a game of double Dutch jump rope – you want to jump in at just the right moment. If you or someone you know is thinking, “What’s the best age to get pregnant when I have PCOS?” then you’ve clicked on the right blog post!
As a nurse and fertility coach, I’m here to help give you information about finding that “sweet spot” age for pregnancy with PCOS. It’s all about understanding your body and making the best decision for you.
What is PCOS?
Polycystic Ovary Syndrome (PCOS) is a common health condition that affects a woman’s hormonal levels, leading to issues with the menstrual cycle, fertility, and reproductive health. PCOS is characterized by hormonal imbalances and the presence of small cysts on the ovaries.
This hormonal imbalance interferes with the regular release of eggs from the ovaries, often causing irregular or absent periods. Women with PCOS may experience symptoms such as acne, excessive hair growth (hirsutism), weight gain, and thinning hair.
The diagnostic criteria may include irregular menstrual cycles, elevated levels of androgen hormones, and ultrasound findings of polycystic ovaries. These factors contribute to fertility challenges, making it harder for women with PCOS to conceive.
Seeking medical advice and early intervention are crucial in managing PCOS and its impact on reproductive health.
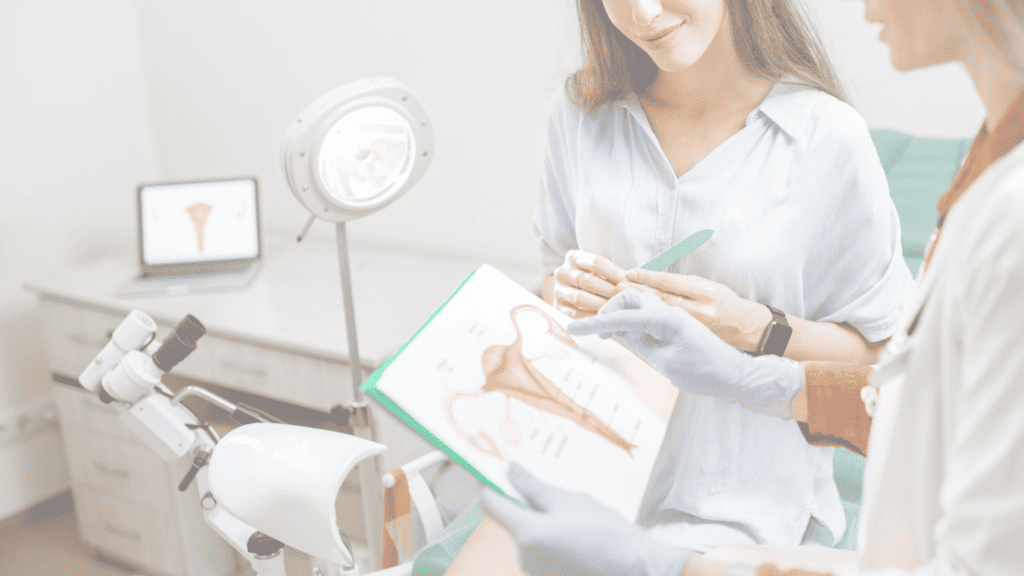
How Does PCOS Affect Fertility?
PCOS can significantly impact fertility by disrupting ovulation, which is essential for conceiving. The hormonal imbalances associated with PCOS can lead to irregular or absent ovulation, making it challenging for women with PCOS to get pregnant.
Ovulatory dysfunction is a common feature of PCOS, where the ovaries may not release eggs regularly or may not release them at all due to the excess production of androgens. This irregular ovulation pattern greatly reduces the chances of conception.
Ovulation plays a crucial role in the menstrual cycle as it marks the release of a mature egg from the ovary, which needs to be fertilized by sperm for pregnancy to occur. Hormonal regulation is essential for the proper functioning of the reproductive system, and disruptions in these hormonal levels can further complicate infertility in women with PCOS.
What Are the Risks of Getting Pregnant with PCOS?
Women with PCOS who get pregnant may face certain risks and health complications that require careful monitoring and medical intervention. These risks can affect both the mother’s and baby’s health during pregnancy.
One significant risk for pregnant women with PCOS is an increased likelihood of developing gestational diabetes, a condition that can lead to complications such as high blood pressure and preeclampsia.
PCOS can contribute to an increased risk of miscarriage or premature birth. Maternal health concerns include the potential for developing pregnancy-induced hypertension and an elevated risk of cesarean section delivery. These factors highlight the importance of regular prenatal care and specialized monitoring to ensure the well-being of both the mother and the developing fetus.
Gestational Diabetes
Gestational diabetes, a common complication of pregnancy in women with PCOS, requires close monitoring and management to prevent adverse effects on both the mother and the baby. Untreated gestational diabetes can lead to long-term health issues and increase the risk of maternal mortality.
The presence of gestational diabetes in pregnant women with PCOS can heighten the likelihood of various pregnancy complications, such as preeclampsia, preterm birth, and macrosomia (large birth weight). These complications not only pose risks to the health of the mother but can also impact the well-being of the developing fetus. Effective management of gestational diabetes through dietary strategies, regular blood sugar monitoring, and, if necessary, insulin therapy is crucial to mitigate these risks and promote a healthier pregnancy outcome.
Preeclampsia
Preeclampsia, a serious condition characterized by high blood pressure during pregnancy, poses risks to both the mother’s and baby’s health. Women with PCOS may have an increased likelihood of developing preeclampsia, requiring vigilant monitoring and medical interventions for maternal wellness.
This connection between PCOS and preeclampsia underscores the importance of understanding how one condition can impact the other during pregnancy. High blood pressure in pregnancy can lead to various complications such as preterm birth, low birth weight, and even life-threatening situations for the mother. Therefore, maintaining maternal wellness by managing blood pressure levels through regular check-ups, proper prenatal care, and a healthy lifestyle is crucial in reducing the risks associated with these pregnancy-related conditions.
Miscarriage
Miscarriage, the loss of a pregnancy before 20 weeks, is a concern for women with PCOS due to hormonal imbalances and other factors affecting pregnancy. Dealing with the emotional toll of miscarriage is essential for the well-being and mental health of women with PCOS.
The challenges of fertility in women with PCOS are multifaceted, with factors such as irregular menstrual cycles, ovulation issues, and insulin resistance playing a role. These complexities can make conception more difficult, increasing the risk of miscarriage.
Addressing emotional well-being is crucial during this journey, as the stress and anxiety of fertility struggles can further impact hormonal balance and reproductive health. Support systems, including counseling, support groups, and open communication with partners, are vital in providing the necessary emotional support to navigate the ups and downs of the fertility process.

What is the Best Age to Get Pregnant with PCOS?
Determining the best age to get pregnant with PCOS involves considering factors such as maternal age, fertility trends, and pregnancy success rates. Age plays a crucial role in fertility and pregnancy outcomes for women with PCOS.
Younger women with PCOS generally have better fertility rates compared to older women due to the age-related decline in egg quality. Maternal age also impacts the risk of pregnancy complications, such as gestational diabetes and hypertension.
Research suggests that women with PCOS who conceive at a younger age may have a higher likelihood of successful pregnancy outcomes. Advanced maternal age can pose challenges for conception and increase the risk of miscarriage in women with PCOS.
It is important for women with PCOS to discuss their fertility goals with healthcare providers and consider age-related factors when planning for pregnancy.
Age and PCOS Symptoms
The age factor can influence the severity of PCOS symptoms, hormonal imbalances, and ovulatory dysfunction. As women with PCOS age, the impact of the condition on fertility and reproductive health may vary.
As women progress through different life stages, the hormonal regulation within their bodies evolves, affecting the manifestation of PCOS symptoms. Younger women with PCOS often experience heightened androgen levels, leading to irregular menstrual cycles and potential fertility challenges.
As women age, their hormone levels may fluctuate, impacting the frequency and intensity of ovulatory dysfunction. This interplay between age and hormonal balance underscores the complexity of PCOS management, highlighting the need for personalized treatment approaches that consider individual factors such as age-related changes in ovulation patterns.
Age and Fertility
Age is a critical factor in the fertility journey of women with PCOS, impacting ovulation patterns, pregnancy risks, and the need for close ovulation monitoring. Advancing maternal age can present unique challenges and considerations for women with PCOS.
As women with PCOS age, their fertility may further decline due to ovulatory dysfunction, complicating the process of conception. Ovulation monitoring becomes increasingly important to track fertile windows accurately. Pregnancy risks, such as gestational diabetes and preeclampsia, tend to rise with maternal age in women with PCOS. The impact of age on reproductive outcomes underscores the importance of early intervention and personalized fertility treatments tailored to individual needs and circumstances.
Age and Pregnancy Risks
Maternal age influences the risks associated with pregnancy in women with PCOS, including factors like gestational diabetes, preeclampsia, and high blood pressure. Understanding how age impacts pregnancy risks is crucial for maternal health.
Older women with PCOS face an increased likelihood of experiencing complications during pregnancy. Advanced maternal age is often linked to higher rates of gestational diabetes, which can pose risks to both the mother and baby. Similarly, older women with PCOS are at a heightened risk of developing conditions such as high blood pressure and preeclampsia, which can have serious implications for pregnancy outcomes.
To mitigate these risks, close monitoring and tailored interventions are essential for maintaining maternal wellness and ensuring positive pregnancy outcomes.

Can Women with PCOS Have a Successful Pregnancy?
Women with PCOS can achieve successful pregnancies through a combination of lifestyle changes, medical treatments, and assisted reproductive technologies. With the right interventions, women with PCOS can increase their chances of conceiving and having a healthy pregnancy.
Effective lifestyle modifications for women with PCOS include maintaining a balanced diet, regular exercise routine, and managing stress levels, which can help regulate hormones and improve overall fertility. Certain medications such as clomiphene citrate or letrozole may be prescribed to induce ovulation. In cases where these options are not successful, fertility treatments like intrauterine insemination (IUI) or in vitro fertilization (IVF) can be considered to maximize the chances of successful conception. It’s essential for women with PCOS to work closely with their healthcare provider to tailor a personalized plan for achieving pregnancy.
Lifestyle Changes
Implementing lifestyle changes, such as maintaining a healthy diet, regular exercise, and stress management, can positively impact the fertility and overall health of women with PCOS. These modifications can enhance reproductive outcomes and support maternal well-being.
A balanced diet rich in fruits, vegetables, whole grains, and lean proteins can help regulate hormones and improve insulin sensitivity, which is crucial for women with PCOS.
Engaging in physical activity, like aerobic exercises and strength training, not only aids in weight management but also reduces insulin resistance.
Stress reduction techniques such as mindfulness, prayer, and meditation can lower cortisol levels and optimize reproductive function.
Achieving and maintaining a healthy body weight through these lifestyle changes can significantly improve fertility outcomes for women dealing with PCOS.
Medications
Medical interventions, including hormonal therapy and medications like Metformin and Clomid, can help women with PCOS regulate their menstrual cycles, improve ovulation, and increase their chances of successful conception. These treatments play a vital role in managing PCOS-related fertility issues.
Metformin, a medication typically used to manage type 2 diabetes, has also been found effective in treating PCOS by addressing insulin resistance, a common issue in women with the condition. By lowering insulin levels, Metformin helps restore hormonal balance, leading to more regular ovulation.
Clomid, on the other hand, is a medication that stimulates ovulation in women who do not ovulate regularly on their own. It works by triggering the release of hormones necessary for the development and release of mature eggs, increasing the likelihood of conception.
As always, make sure to consult with your doctor on any medications along your fertility journey.
Assisted Reproductive Technology (ART)
Assisted Reproductive Technology (ART) procedures like In Vitro Fertilization (IVF), involving techniques such as egg retrieval and embryo transfer, offer viable options for women with PCOS facing fertility challenges. ART can significantly improve the chances of successful pregnancy for women with PCOS.
Fertility specialists play a crucial role in guiding women with PCOS through the various stages of ART procedures, from initial consultations to monitoring and support throughout the process. Through personalized treatment plans, these specialists can optimize the chances of successful embryo implantation and pregnancy. Techniques like ovarian stimulation and monitoring are tailored to individual needs, ensuring the best possible outcomes. Advancements in reproductive technologies continue to enhance the efficacy and safety of ART procedures, providing hope and options for women with PCOS seeking to start a family.

What Are the Challenges of Getting Pregnant with PCOS?
Women with PCOS may encounter various challenges when trying to conceive, including irregular menstrual cycles, hormonal imbalances, and difficulty predicting ovulation. These factors can complicate the fertility journey for women with PCOS.
Irregular menstruation, a common symptom of PCOS, causes irregular ovulation, making it challenging for women to pinpoint their most fertile days. The hormonal imbalances characteristic of PCOS can disrupt the delicate interplay necessary for successful conception. The ovulation difficulties often experienced by women with PCOS further hinder their chances of getting pregnant naturally. These combined factors create a complex landscape for those with ovulatory dysfunction seeking to embark on the path to motherhood.
Irregular Menstrual Cycles
Irregular menstrual cycles, a common symptom of PCOS, can be a significant challenge for women trying to conceive. Anovulation, or the lack of ovulation, contributes to irregularities in the menstrual cycle, affecting fertility.
This lack of ovulation in women with PCOS can lead to unpredictable and inconsistent menstrual cycles, making it difficult to pinpoint the fertile window essential for conception. Menstrual irregularities, such as prolonged or absent periods, further complicate the process of tracking ovulation and timing intercourse for optimal chances of pregnancy.
Understanding these patterns and disruptions in the menstrual cycle is crucial for women with PCOS who are actively seeking to conceive, as it guides them in seeking appropriate medical interventions and fertility treatments.
Hormonal Imbalances
Hormonal imbalances, particularly in insulin sensitivity and hormone levels, can disrupt the reproductive functions of women with PCOS. These imbalances may affect ovulation, menstrual regularity, and overall fertility.
Irregular ovulation makes it challenging for women with PCOS to conceive. The hormonal fluctuations can lead to irregular menstrual cycles, making it difficult to predict the fertile window. In PCOS, the excess androgens produced can further disrupt the delicate balance of hormones crucial for reproductive health. Understanding these complex interactions is vital in managing fertility challenges associated with hormonal imbalances in women with PCOS.
Difficulty Predicting Ovulation
The irregularities in ovulation patterns make it challenging for women with PCOS to predict fertile windows and timing for conception. Ovulation monitoring and techniques like follicle stimulation may be necessary to enhance the chances of successful pregnancy.
Women with PCOS often struggle with identifying ovulation signs due to hormonal fluctuations, leading to uncertainty in determining the most fertile days. In such cases, methods such as basal body temperature tracking, ovulation predictor kits, and cervical mucus monitoring can aid in pinpointing ovulation.
Follicle stimulation through medications like Clomid or injections may be prescribed by healthcare providers to induce ovulation. By combining these methods with fertility awareness practices, women with PCOS can improve their chances of conceiving naturally.

What Are the Precautions to Take When Trying to Get Pregnant with PCOS?
When trying to conceive with PCOS, it is crucial to take specific precautions to optimize fertility outcomes. Preconception care, ovulation induction, and the use of supplements like folic acid can enhance the chances of successful conception for women with PCOS.
In addition to these measures, it is also important for women with PCOS to focus on maintaining a healthy lifestyle, including regular exercise and a balanced diet. Weight management plays a significant role in fertility for women with PCOS, as excess weight can impact hormone levels and ovulation. Seeking the guidance of healthcare professionals specializing in fertility and maternal health education can provide tailored strategies for maximizing the chances of a successful pregnancy.
By taking proactive steps towards preconception care, women with PCOS can improve their overall reproductive health and increase the likelihood of achieving their goal of conceiving.
Maintain a Healthy Weight
Maintaining a healthy weight through proper weight management, including monitoring Body Mass Index (BMI) and focusing on weight loss if necessary, can positively impact fertility and reproductive health outcomes for women with PCOS.
Research has shown that women with PCOS who are overweight or obese often experience hormonal imbalances that can disrupt ovulation and menstrual cycles, affecting their ability to conceive. By adopting lifestyle modifications such as regular exercise and a balanced diet, individuals with PCOS can not only improve their BMI but also enhance their chances of successful conception. Weight loss can help reduce insulin resistance, which is a common issue in PCOS and can further improve fertility outcomes.
Monitor Blood Sugar Levels
Regularly monitoring blood sugar levels and addressing insulin sensitivity through lifestyle changes are essential steps for women with PCOS trying to conceive. Maintaining stable blood sugar levels can support overall health and fertility.
- One of the key factors in managing insulin resistance in PCOS is adopting a balanced diet rich in whole foods, low in refined sugars, and high in fiber. This can help stabilize blood sugar levels and improve insulin sensitivity, which are crucial for reproductive health.
Incorporating regular physical activity into daily routines can further enhance insulin sensitivity and support metabolic function. By making these proactive lifestyle changes, women with PCOS can positively impact their metabolic health, potentially improving their chances of successful conception and healthier pregnancies.
Work with a Fertility Specialist
Seeking guidance from a fertility specialist or gynecologist is crucial for women with PCOS planning to conceive. A fertility specialist can provide medical consultations, monitor ovulation, and recommend appropriate treatments to enhance fertility outcomes.
During fertility consultations, specialists thoroughly assess the individual’s reproductive health, hormone levels, and any underlying conditions affecting fertility.
Ovulation induction methods such as medications or procedures like intrauterine insemination (IUI) may be suggested to regulate ovulation and improve chances of conception.
Treatment options for PCOS-related fertility issues may include lifestyle modifications, medications to manage symptoms, and assisted reproductive technologies like in vitro fertilization (IVF) for those facing more complex infertility challenges.
Wrapping up our chat about finding the best age to get pregnant with PCOS, it’s clear that there’s no one-size-fits-all answer. However, what stands out is the importance of focusing on improving your overall health.
This not just nudges the odds of related fertility issues in your favor, but it also paves the way for a smoother PCOS and pregnancy journey. Success in this arena often comes from understanding your body, partnering closely with your healthcare provider, and making lifestyle choices that boost your health.
Remember, every step you take towards better health is a step closer to enhancing your pregnancy success with PCOS. Whether you’re just starting to think about pregnancy or you’re already on this path, know that you’re not alone.
Together, let’s embrace the journey, armed with knowledge, support, and a strong focus on health. Here’s to your success, your health, and your future!

Octavia Steen is an NBDA certified fertility doula, health coach, certified fitness nutrition specialist, aspiring missionary with the COGIC, and owner of Mother Mindset. She helps future and current mamas become more consistent in faith + fitness and grow closer to God so they can create a healthier lifestyle from the inside out!






